The average nursing home can be depressingly institutional. For the growing number of people suffering from dementia, these facilities are even worse: Their repetitive architecture makes it easy to get lost, and they look nothing like the places where patients have lived their entire lives. The Copenhagen-based firm Nord Architects is building a series of centers for patients with Alzheimer’s and dementia that feel more like villages or cities, rather than bleak institutions.
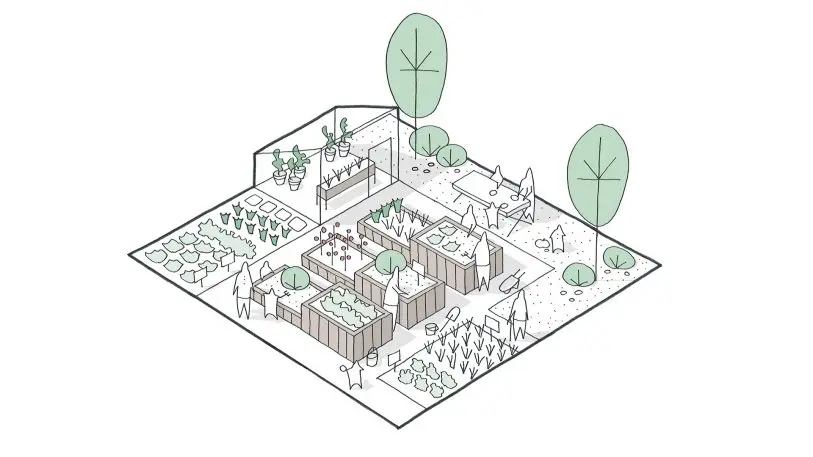
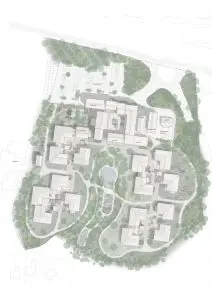
“We know most of the patients come from these types of villages,” says Morten Gregersen, a partner at Nord who led the design. “We wanted to create an environment that wasn’t alien to the normal place they come from. It’s very much about creating a noninstitutional atmosphere that is based on the traditions of the local architectural works.”
Since residents are already dealing with a debilitating disease that makes them forgetful, being in an environment that’s similar to what they’re used to could ease the transition from living at home to living in a care-taking facility. “As their cognitive level slowly degenerates and their ability to read new things disappears, they relate to things they know much better, and things they knew in their childhood,” Gregersen says. “All of these things need to be incorporated into the design so we don’t create [places] where people get lost and confused.”
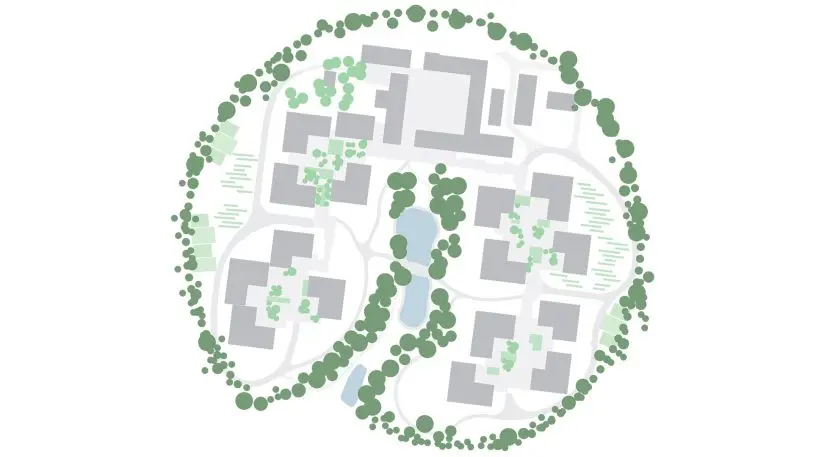
There’s a reason that most medical facilities aren’t designed like this. Big, modern buildings make it logistically easier to care for more people more efficiently since they’re all located physically much closer to each other. Along with creating a place that felt more like a village, this was another important consideration during the design process for Alzheimer’s Village. To make it easier for staff to care for patients, their living quarters are incorporated into the village itself. Plus, Gregersen hopes that because the environment will be so much better for the patients, they’ll require less day-to-day care.
He and his team looked into research about how a patient’s surroundings can impact their day-to-day quality of life and recovery. One example? “In a neurological hospital, the most important thing in a patient’s room with brain damage is they need to be exposed to daylight as much as possible,” Gregersen says. Though a recent study published earlier this summer after the master design was finished disputes the effectiveness of this, Gregersen’s approach–to use research-backed evidence to influence the design of healthcare spaces–is sound. “We try to use architectural ways of solving things instead of institutional, machine-like, or normative ways of thinking about healthcare buildings,” he says.
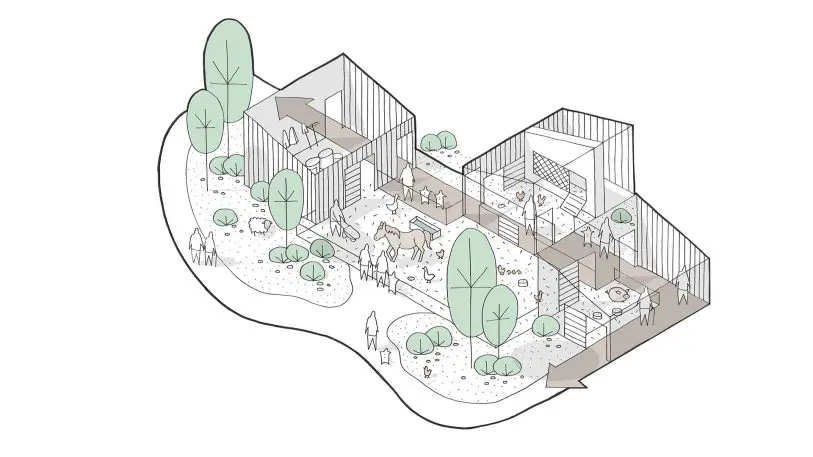
“Before institutions became very modern in the ’60s and ’70s, we took care of sick people in small community-like places,” Gregersen says. “Our families took care of their old people. It’s going back to how we did it before we institutionalized our way of treating elderly.”
That project is still in planning stages, so it’s hard to say how it will function more practically. But it’s a much more human way of thinking about how to care for elderly people with Alzheimer’s and dementia. “You don’t use fences, but create an atmosphere where people take care of each other,” Gregersen says.
Recognize your brand’s excellence by applying to this year’s Brands That Matter Awards before the early-rate deadline, May 3.







